Difference between revisions of "Nasopharyngeal swab"
Shawndouglas (talk | contribs) (Created as needed.) |
(No difference)
|
Latest revision as of 19:57, 25 March 2020
| Nasopharyngeal swab | |
|---|---|
 Nasopharyngeal swab | |
| Purpose | Diagnosis of certain viral infections |
| MedlinePlus | 003747 |
A nasopharyngeal swab is a device used for collecting a sample of nasal secretions from the back of the nose and throat.[1][2] The sample is then analyzed for the presence of organisms or other clinical markers for disease. This diagnostic method is commonly used in suspected cases of whooping cough, diphtheria, influenza, and various types of diseases caused by the coronavirus family of viruses, including SARS, MERS, and COVID-19.[3][4][5][6][7][8]
Procedure
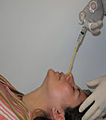
To collect the sample, the swab is inserted in the nostril and gently moved forward into the nasopharynx, a region of the pharynx that covers the roof of the mouth.[9] The swab is then rotated for a specified period of time to collect secretions, then the swab is removed and placed into a sterile viral transport media, which preserves the sample for the subsequent analysis.[5][6]
Material composition of swab
Similar in concept to the cotton swab, a swab used for nasopharyngeal collection constitutes a narrow stick made of a short plastic rod that is covered, at one tip, with adsorbing material such as cotton, polyester, or flocked nylon. (Some swab handles have been made of nichrome or stainless steel wire.[3][10]) The swab material used for a particular diagnostic application may vary based on the test type. Some research has shown that flocked swabs collect a larger volume of the sample material, when compared to fiber swabs.[7][11]
Related methods
Slightly different but related is nasopharyngeal aspiration. Rather than depending on a physical swab to catch material from the nasopharynx, aspiration uses a catheter that is attached to a syringe. As with the swab method, the catheter is placed into the nostril and gently advanced to the nasopharynx, where approximately one to three milliliters of saline are introduced, followed by immediate re-aspiration of the saline—along with cells and secretions—back into the syringe.[7] This aspiration method is often used when 1. the patient is an infant or elderly and 2. when the method is indicated as effective for a test type.[6][12]
Diagrams
-
Diagram of the nasal cavity
-
Nasopharyngeal aspiration
-
Collecting nasopharyngeal aspirate
-
Video of a nasopharyngeal swab test for COVID-19
See also
References
- ^ "Nasopharyngeal culture". MedlinePlus. 23 March 2020. Retrieved 25 March 2020.
- ^ Pavord, T.; Pavord, M. (2004). The complete equine veterinary manual: A comprehensive and instant guide to equine health (2nd ed.). David & Charles. p. 206. ISBN 9780715318836.
- ^ a b Junkins, A. (2010). "20. Identification of Pathogenic Bacteria". In Mukherjee, K.I.; Ghosh, S. (eds.). Medical Laboratory Technology. Vol. 2 (2nd ed.). Tata McGraw-Hill. p. 515. ISBN 9781259000768.
- ^ "Specimen Collection". Pertussis (Whooping Cough). Centers for Disease Control and Prevention. 18 November 2019. Retrieved 25 March 2020.
- ^ a b Irving, S.A.; Vandermause, M.F.; Shay, D.K.; Belongia, E.A. (2012). "Comparison of nasal and nasopharyngeal swabs for influenza detection in adults". Clinical Medicine & Research. 10 (4): 215–8. doi:10.3121/cmr.2012.1084. PMC 3494547. PMID 22723469.
- ^ a b c "Influenza Specimen Collection" (PDF). Centers for Disease Control and Prevention. n.d. Retrieved 25 March 2020.
A nasopharyngeal (NP) swab is the optimal upper respiratory tract specimen collection method for influenza testing.
- ^ a b c McPherson, R.A.; Pincus, M.R. (2017). Henry's Clinical Diagnosis and Management by Laboratory Methods (First South Asia ed.). Elsevier. p. 1083. ISBN 9788131231272.
- ^ World Health Organization (19 March 2020). "Laboratory testing for coronavirus disease (COVID-19) in suspected human cases: Interim guidance, 19 March 2020". WHO/COVID-19/laboratory/2020.5. World Health Organization. hdl:10665/331501. Retrieved 25 March 2020.
- ^ Marty FM, Chen K, Verrill KA (28 May 2020). "How to Obtain a Nasopharyngeal Swab Specimen". The New England Journal of Medicine. 382 (22): e76. doi:10.1056/NEJMvcm2010260. PMID 32302471.
- ^ Gritzfeld, J.F.; Roberts, P.; Roche, L.; et al. (2011). "Comparison between nasopharyngeal swab and nasal wash, using culture and PCR, in the detection of potential respiratory pathogens". BMC Research Notes. 4. 122. doi:10.1186/1756-0500-4-122. PMC 3084159. PMID 21489228.
- ^ Sing, S.K., ed. (2014). Human Respiratory Viral Infections. CRC Press. p. 166. ISBN 9781466583207.
- ^ Nunes, M.C.; Soofie, N.; Downs, S.; et al. (2016). "Comparing the Yield of Nasopharyngeal Swabs, Nasal Aspirates, and Induced Sputum for Detection of Bordetella pertussis in Hospitalized Infants". Clinical Infectious Diseases. 63 (Suppl. 4): S181–S186. doi:10.1093/cid/ciw521. PMC 5106614. PMID 27838671.
Notes
This article is a direct transclusion of the Wikipedia article and therefore may not meet the same editing standards as LIMSwiki.