Journal:Anatomic pathology quality assurance: Developing an LIS-based tracking and documentation module for intradepartmental consultations
| Full article title | Anatomic pathology quality assurance: Developing an LIS-based tracking and documentation module for intradepartmental consultations |
|---|---|
| Journal | Journal of Pathology Informatics |
| Author(s) | Dundar, Bilge; Chen, Stephanie J.; Blau, John L.; Anand Rajan, K.D.; Samuelson, Megan I.; Greek-Lippe, Michelle L.; Lake, Kim S.; Robinson, Robert A. |
| Author affiliation(s) | University of Iowa Hospitals and Clinics |
| Primary contact | bilge-dundar at uiowa dot edu |
| Year published | 2022 |
| Volume and issue | 13 |
| Article # | 100109 |
| DOI | 10.1016/j.jpi.2022.100109 |
| ISSN | 2153-3539 |
| Distribution license | Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International |
| Website | https://www.sciencedirect.com/science/article/pii/S2153353922007039 |
| Download | https://www.sciencedirect.com/science/article/pii/S2153353922007039/pdfft (PDF) |
Abstract
Background: An electronic intradepartmental consultation system for anatomic pathology (AP) was conceived and developed in the laboratory information system (LIS) of University of Iowa Hospitals and Clinics in 2019. Previously, all surgical pathology intradepartmental consultative activities were initiated and documented with paper forms, which were circulated with the pertinent microscopic slides and were eventually filed. In this study, we discuss the implementation and utilization of an electronic intradepartmental AP consultation system.
Methods: Workflows and procedures were developed to organize intradepartmental surgical pathology consultations from the beginning to the end point of the consultative activities entirely using a paperless system that resided in the LIS.
Results: The electronic consult system allowed electronic documentation of all steps of intradepartmental consultative activities. The system provided a tracking ability for consulted cases and improved access to consult discussion for all departmental personnel, staff, and trainees. A consultation work queue was created for each pathologist, and a summary of individual consultative workload was made possible. Documentation of anatomic pathology quality assurance for intradepartmental consultative activity was easily assessed.
Conclusions: The electronic intradepartmental consult system has allowed our department to electronically track intradepartmental consult cases, store the consultative opinion text with the case, record the pathologists involved, and document the consultation for internal quality assurance review, as well as for accrediting organizations. Summarization of pathologist workload related to consultative activity was quantifiable, and optimization of the consultative process was maximized for education in an academic setting.
Keywords: electronic intradepartmental consultation, anatomic pathology, surgical pathology, laboratory information system
Introduction
Although relatively recent, the benefit of electronic consultation (e-consultation) has been noted across the spectrum in medicine. In the clinical setting, the availability of such consultation has decreased patient waiting times for specialist consultation and has had a particularly positive effect in patient populations that are underserved.[1][2] Surgical specialties have also noted increased efficiency in scheduling surgical intervention in their waiting lists when utilizing e-consultation.[3]
In anatomic pathology (AP), it has been shown that intra‐departmental consultations increase the value and diagnostic accuracy of reports and are vital steps to improve patient care.[4][5][6] However, while consultation in AP is long established, e-consultation is less well established.
The University of Iowa Hospitals and Clinics sought to improve its tracking and documentation process for AP intradepartmental consultations by using its laboratory information system (LIS), AP Beaker, in 2019. In this study, we describe the development, implementation, and utilization of an electronic intradepartmental AP consultation system and discuss its advantages and disadvantages.
Background
Institutional details and historical context of paper-based intradepartmental consultations
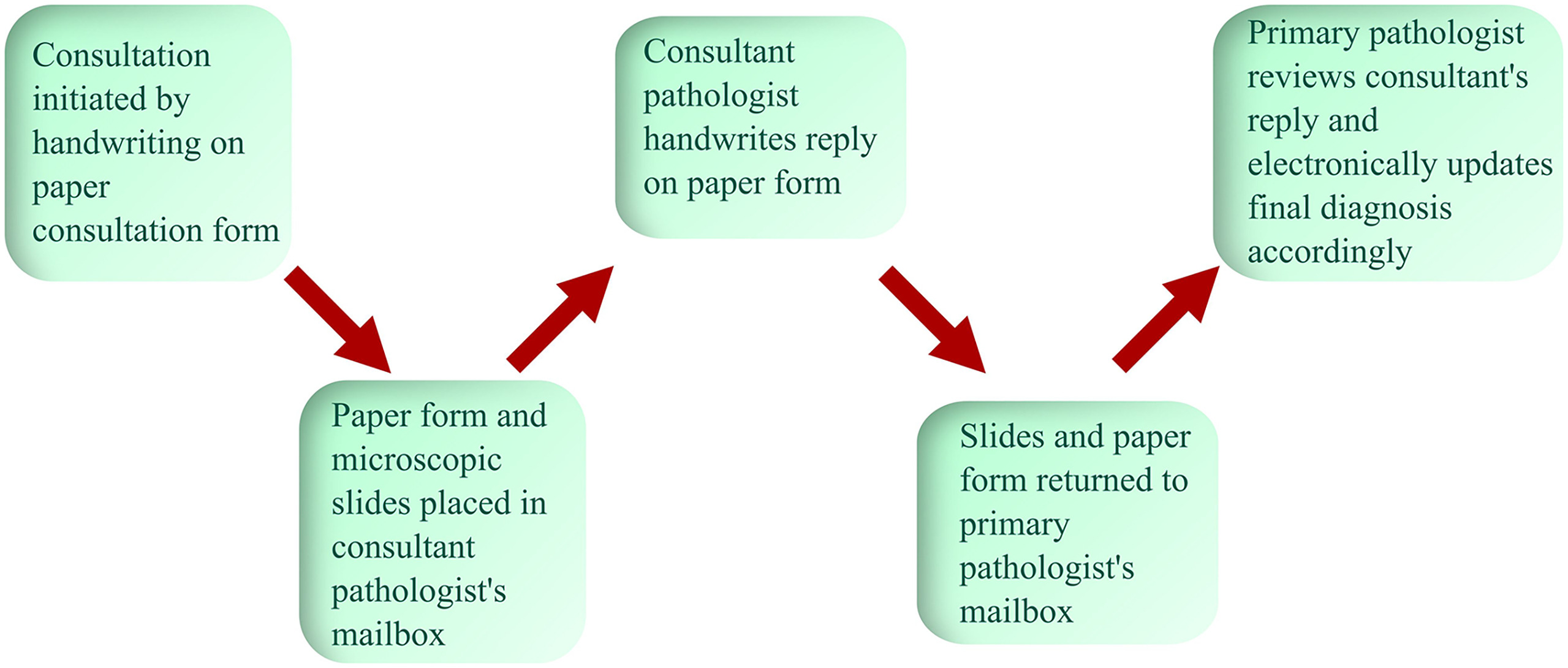
The Department of Pathology at our institution is a mid-sized academic pathology program (presently 36 clinical faculty, 20 residents, nine fellows) with a partially subspecialized service model in anatomic pathology, including renal pathology, hematopathology, dermatopathology, and neuropathology serving as dedicated subspecialty services. Gastrointestinal pathology and cytopathology services are essentially subspecialized. Prior to converting to an electronic form of consultation in AP, a long-standing paper system was in place and utilized despite the implementation of a now legacy electronic LIS (Cerner Corporation's PathNet) several decades ago and of the current AP LIS (Epic Systems Corporation's AP Beaker), which went live in 2015. Neither LIS had modules to implement or store intradepartmental consultation discussions and did not allow intradepartmental consultations to be performed electronically. In the paper-based workflow, an 8.5 x 11-inch form was colored yellow to stand out from other forms and reports (Fig. 1). Consultations were initiated by handwriting on the paper form. These consultation forms were placed with the slides and directed to the consultant faculty, who in turn wrote their consultative thoughts and returned the sheet with the slides to the primary pathologist (Fig. 2). The primary pathologist recorded the consulting pathologist in the final report in a dedicated data field in the LIS.
|
|
Methods
Implementation of electronic intradepartmental consultations
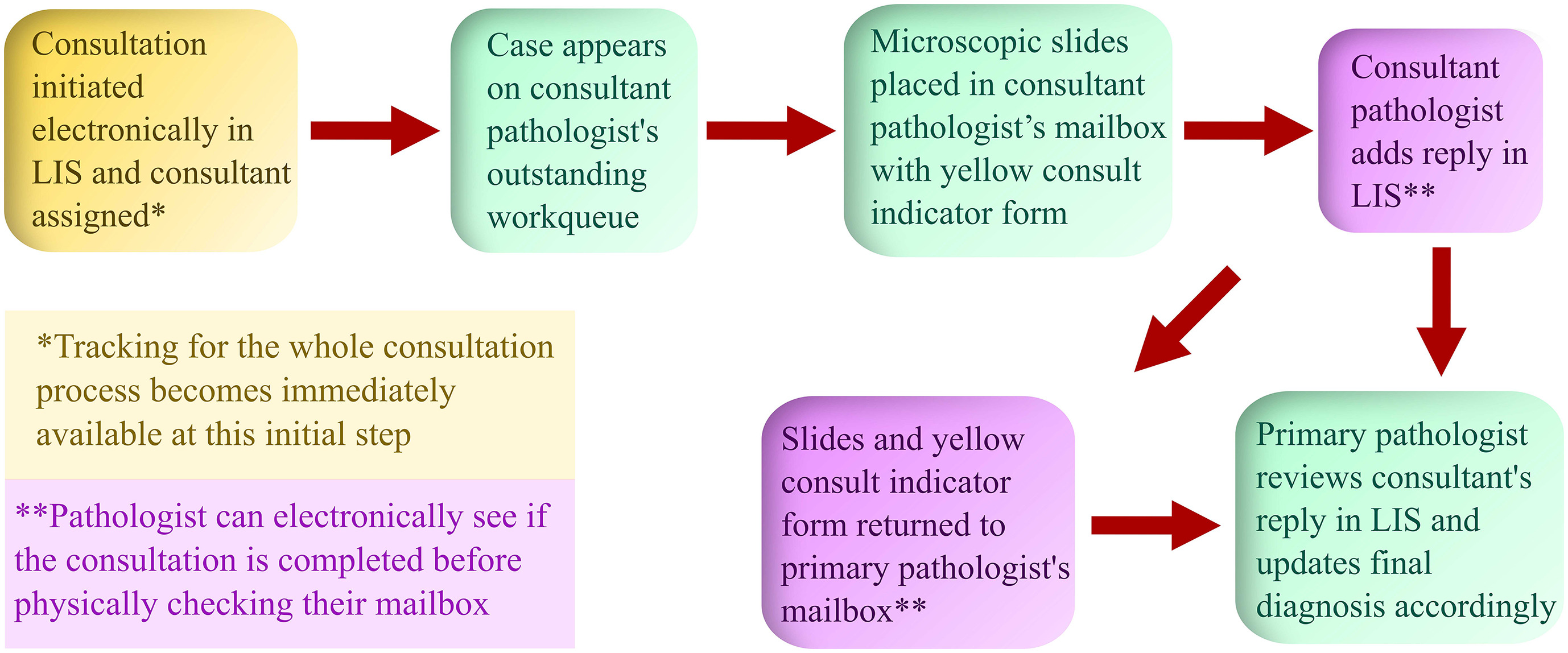
On September 1, 2019, intradepartmental consultations transitioned to an electronic format in the LIS, with the functionality centered around two data fields: "Internal consultation discussion" and "Consultants." The implemented electronic workflow is diagramed in Fig. 3.
|
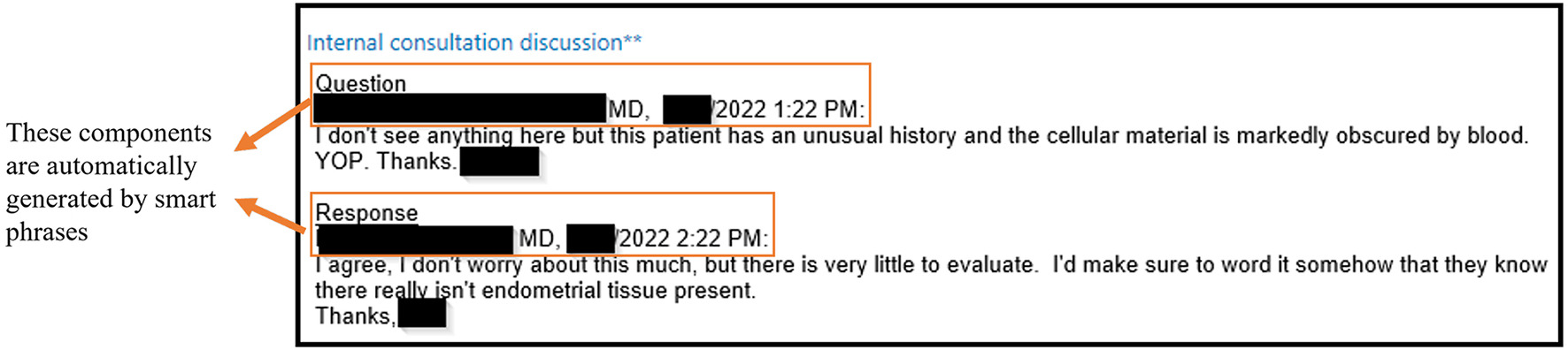
In the electronic system, the primary pathologist initiates the consultation process by entering information in a field designated "Internal consultation discussion." First, essential information for consultation, namely the primary pathologist’s name, date, and time, is automatically generated by using a smart dot phrase. The primary pathologist then enters the consult question followed by any additional information they would like to provide to the consultant pathologist (Fig. 4).
|
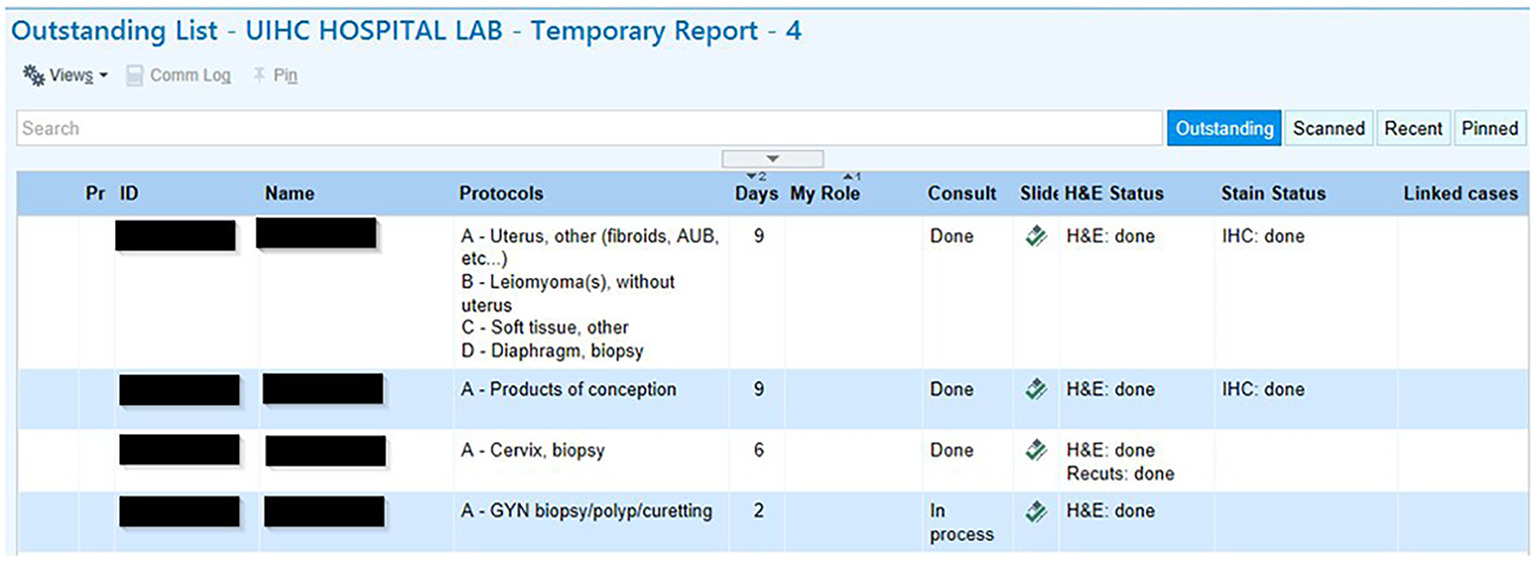
Text from an electronic medical record can be copied and pasted directly into the discussion with any relevant digital images (e.g., endoscopic and radiologic images, gross photos, etc.). The primary pathologist then assigns the consultant pathologist to the case, which results in the case appearing on the consultant’s outstanding work queue as a designated consult (Fig. 5).
|
This is followed by delivery of the relevant microscopic slides and any associated paperwork to the consultant pathologist’s departmental mailbox, along with a reusable 8.5 x 11-inch cardstock consult indicator. This consult indicator, reminiscent of the previous system, is also colored yellow and is used to visually alert the pathologist that there is a consult in their mailbox. The consultant similarly begins their response in the "Internal consultation discussion" text box by inserting a smart dot phrase which automatically generates his/her name, the date, and time. This is followed by entering their reply to the primary pathologist’s question (Fig. 4). The slides and any associated paperwork are then delivered back to the primary pathologist’s mailbox. The system allows multiple pathologists to be asynchronously involved in the consultation discussion, if necessary. For these cases, the primary pathologist may assign additional consultants to the case after the initial consultation. Alternatively, the consultant pathologist may also assign the case to another consultant if they believe an additional opinion would be useful. Relevant microscopic slides and consult indicator form are then delivered to any additional consultant, followed by the workflow cycle described above.
At sign-out, the primary pathologist or trainee, if involved in the case, generates an automatic statement containing the name of the consultant pathologist(s) by typing a smart dot phrase into the "Consultants" field (Fig. 6). This appears in the finalized pathology report. The full details of the consultation discussion are documented in the "Internal consultation discussion" field. The workflow incorporates a safeguard that prompts the pathologist to document the consultant’s contribution at report finalization. If someone attempts to finalize a report containing text in the "Internal consultation discussion" field without using the consultant’s name, placeholders for missing content are automatically generated in the "Consultants" field, obligating the primary pathologist to review the text in the field. The "Internal consultation discussion" field itself, on the other hand, does not appear in the finalized report but remains visible in AP Beaker even after the case is signed out.
|
Analysis of electronic intradepartmental consultations
We focused on the information gathered during the period of implementation and follow-up under the categories of case volumes with regard to specialty and workload tracking ability for individual pathologists, both as those sending as well as those functioning as consultants.
AP cases accessioned at the Surgical Pathology Gross Laboratory were retrieved from the Epic Clarity data warehouse through the Healthcare Enterprise Decision Intelligence (HEDI) business intelligence tool. These included the groups of general surgical pathology, dermatopathology, hematopathology lymph node, and neuropathology cases. We collected data for one year, starting from the very beginning of the implementation, September 1, 2019, until August 31, 2020.
Data processing and analysis were performed using Microsoft Excel (Microsoft Corporation, 2020) and RStudio (RStudio PBC, Version 1.4.1103) running R 64-bit (4.0.5).
Results
The consultation case volume was 7.3% of total cases. Seventy-five percent of consultations were performed and recorded electronically. The remaining 25% of consultations were performed and recorded using the paper system, as there was a gradual roll out of the process which allowed adjustment to a new workflow for the consultation process.
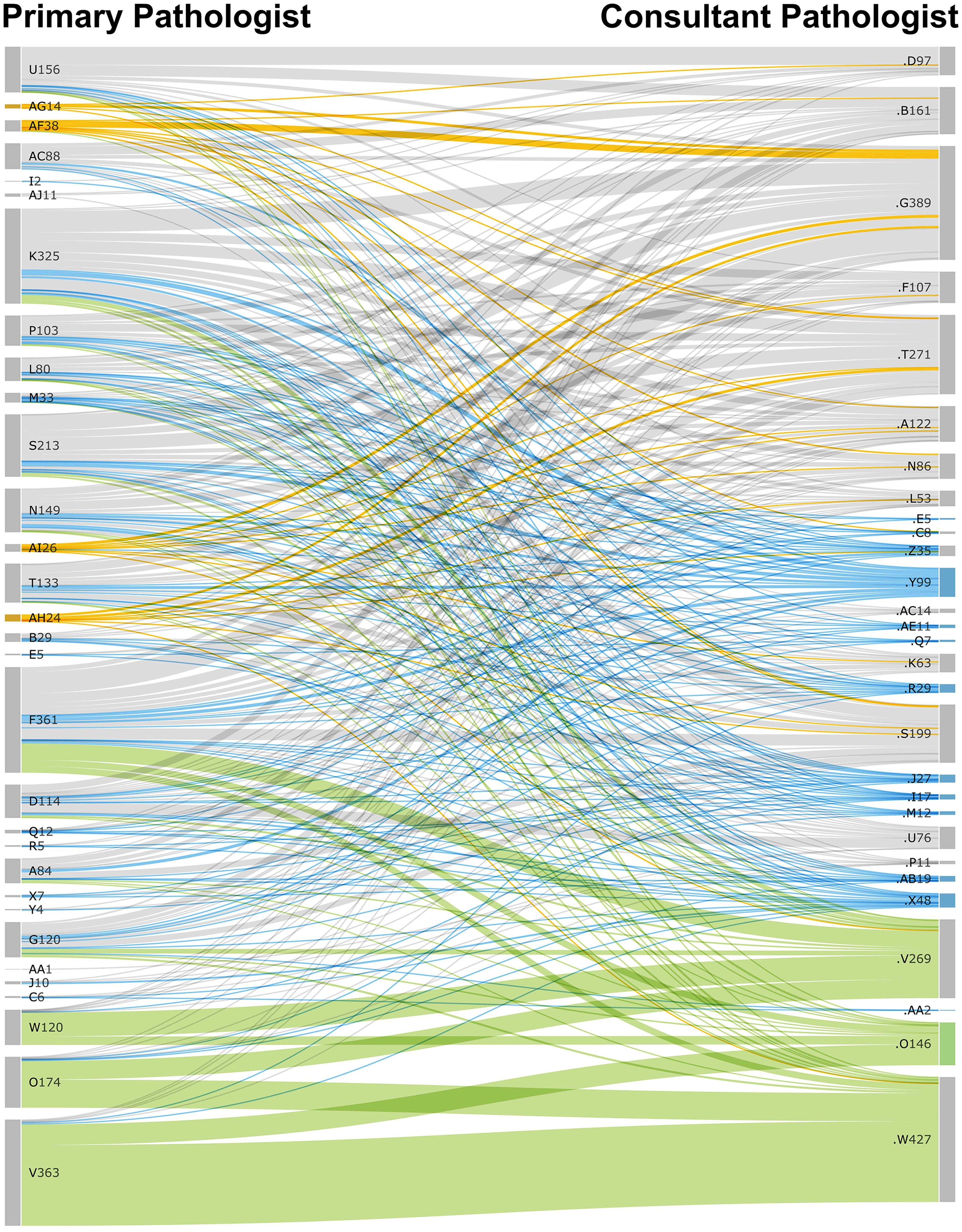
Within 3,049 electronically consulted cases, the majority of consultations (n = 2,852; 93.5%) involved only one consultant; of the remainder, most had two consultants (n = 163; 5.3%) (Table 1). For cases involving multiple consultant pathologists, all consultations were performed asynchronously. Thirty-seven pathologists, consisting of attending pathologists (n = 32) and fellows (n = 5) who had sign-out privileges, sought consultations for their cases. In turn, 29 pathologists had a role as consultants (Fig. 7). Among cases with a single consultant, we broadly classified consults into fellow-originated, dermatopathology-directed, subspecialty-directed, and general surgical pathology (SP) type consults (Fig. 7, Table 2). General SP consults formed 54.8% of all consulted case volume (Table 2). Dermatopathology consults were 29.4% of all consultations (Table 2).
| ||||||||||||||
|
| ||||||||||||||
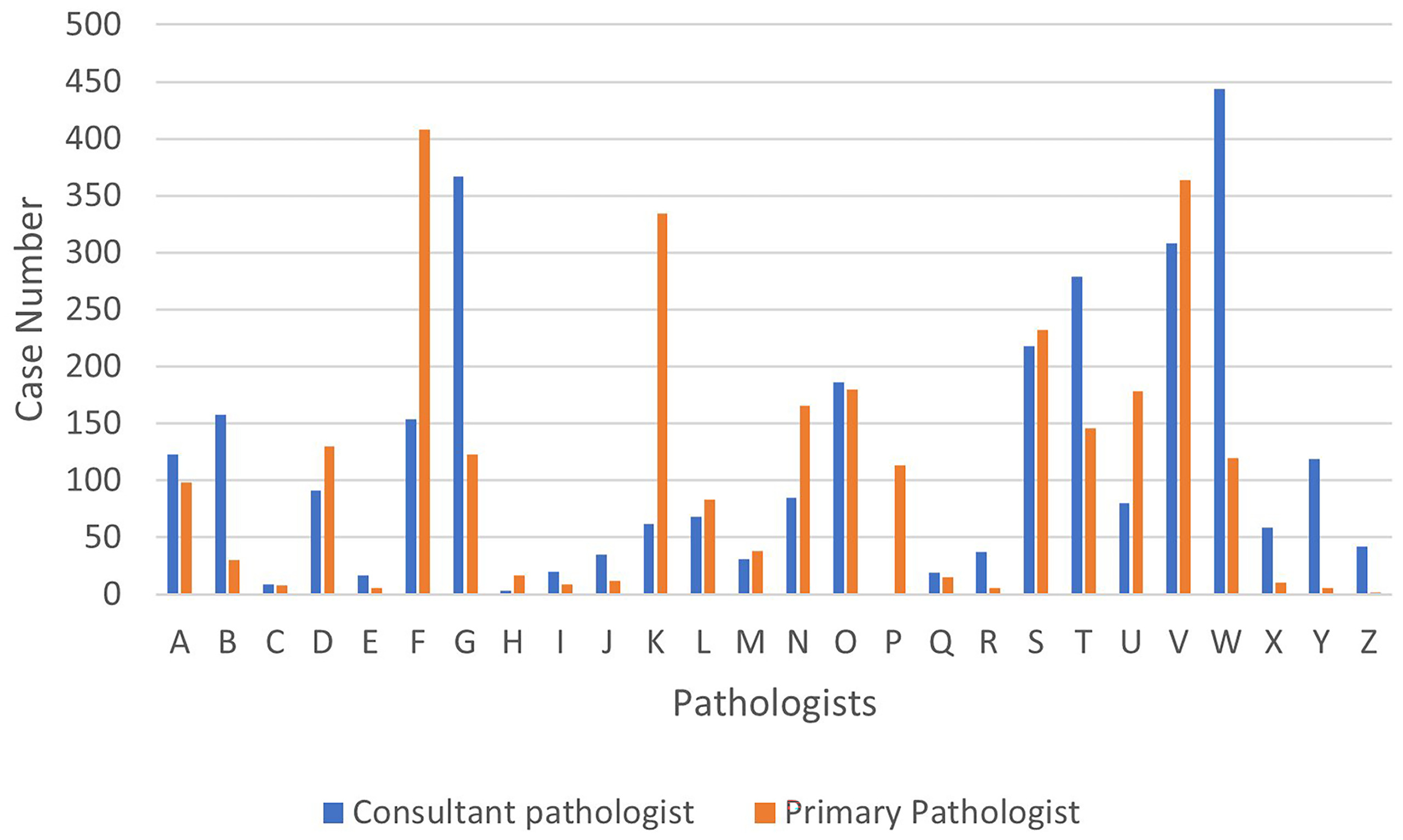
The number of the cases involved in the consultation process for each pathologist are shown in Fig. 8.
|
Department-wide consult case tracking in the electronic consultation process
All laboratory personnel that have access to AP Beaker also have access to the status of the case. Both the primary and consultant pathologists are able to view the cases in their work queue at all times throughout the process (Fig. 5). Clerical personnel are able to locate the case by viewing all steps of consultation in the LIS, a benefit when searching for cases for tumor boards.
In the department, a preliminary diagnosis (hot seat) function is part of the normal workflow for SP and is one of the rotations of the SP fellowship. The preliminary diagnosis fellow handles calls from clinicians, often inquiring about a delay in diagnosis. As the fellow is able to determine that a consultation has been sent, they are able to provide more information about the case.
Optimization of consultations for education in an academic setting
Trainees are involved in the majority of the AP cases in our department. Intradepartmental consultation discussion provides them additional educational opportunities. Anecdotally, we found that being able to see all the steps of consultation provided trainees insight to the approach taken by both general and subspecialty SPs.[5][6] This was not always possible with the previous paper consultation forms, which were filed after finalization of cases and were not easily available for trainees to review. With the current electronic consultation system, the trainees are very frequently involved from the beginning of the consultation process while generating the consultation question. They are able to follow all steps via the LIS and are involved in integrating the consultative opinion in the draft report. As the consultative opinion is stored within the case even after the case is finalized, remaining visible in AP Beaker, the trainees have access to consultative discussion even if they rotate to different services, providing opportunity for educational benefit on follow-up. This is especially helpful when multiple consultant pathologists are asynchronously involved in the process since all consultation discussion is contained within one electronic field.
A further benefit is the availability of consultants’ thought processes to SP fellows, who often are the pathology representative at many tumor boards. The electronic consultation system improved the ability for the fellows to see nuanced considerations that are helpful for making case presentations for tumor boards. This concept is echoed through many other situations for trainees and faculty alike, including review of prior biopsies in preparation for frozen sections on surgical resections, comparison of a patient’s current case to previous samples, and reminding subspecialty pathologists of their own thought processes on difficult cases that resurface over time.
Documentation of pathologists’ consult work
While determining the number of consultations for each pathologist was possible with the previous paper-based consultation system, there were no automated checkpoints to prevent consulted cases from being finalized without documenting the consultation. As such, some cases were inadvertently finalized without formal documentation of consultation in the report. For some of these, consultations were documented in amended reports immediately after the finalization, while others remained undocumented. The nature of the auto-generated text prevents the case from being finalized without documenting the consultation. Furthermore, having the consultant pathologist consistently documented in a discrete data field allows for automated searching that improves detection of underreported workload for pathologists.
Discussion
In a pathology department, the consultation process involves a multi-step circulation of consultation materials within the department, as well as the effective management and documentation of the process. Documenting the details of each consultation is an important task for patient care, for pathologist continuing education through workplace activities, and as a requirement for laboratory accreditation. The College of American Pathologists Master Anatomic Pathology Checklist from 2020 requires that SP laboratories have a "procedure for handling intra- and extra-departmental consultations in the patient’s final report."[7] The ability to track slides and case paperwork traveling between primary pathologist and consultant pathologist is particularly valuable, ideally to provide work queues for consultants and account for pathologists’ time spent on consults.
Consultation in medical practice is important and has been documented to improve overall patient care. Electronic consultation has become more widespread in recent years, extending the benefits of the consultation process.[1][2][3] Consultation in anatomic pathology is an important component of the quality assurance functions in a laboratory and can prevent misdiagnosis. Prior studies in our department, as well as in many others, have shown significant numbers of major diagnostic discrepancies on re-review of pathology reports from other institutions’ pathology departments.[8][9] Given this data, one can readily see the potential benefits of such re-reviews taking place as intradepartmental consultations prior to sign out.
Intradepartmental pathology consultations are conducted in various forms, but little information is available in the published literature regarding these practices. A common method across academic and private practice settings involves face-to-face discussions between the primary pathologist and the consultant across the microscope.[10] Another common practice, owing to demands of time placed on the consultant and a desire to obtain an unbiased and unhurried opinion, involves routing of cases via a trainee or pathologists’ mailbox. In some instances, consultation opinions are verbally rendered and paraphrased into reports from jotted-down notes or memory, possibly an error prone step. A formalized recording of the content of consultation exchanges, however, is not always a part of SP case handling. [10] Intradepartmental consensus case conferences utilizing a multi-headed microscope or a projector is a method of reaching consensus diagnosis by multiple pathologists.[11] Typically, a log record of agreement with diagnoses and those present at the conference is maintained. However, it is uncommon for there to be verbatim capture of the opinions rendered and a granular record of differences in opinion and approaches from the pathologists offering expert opinions in these conferences.
The e-consultation system which we now utilize reduces further the chances of misdiagnosis as the opinions expressed by the consultant are gathered by direct input, rather than by oral "curbside" opinions, handwritten notes, or information transmitted through an intermediary, such as a pathology trainee, all of which are common means for some departments.
In our institution, Epic Systems Corporation's AP Beaker was implemented in 2015; however, it did not have a module to perform intradepartmental consultations electronically. For this reason, a long-standing paper system was in place and utilized, but with many of the problems of a system that is not tied into the LIS and not attached directly to the working draft components of the report.
Consultants did not know what was in their consultant work queue without walking to their mailbox to see the slides, whereas the electronic system allows pathologists to check their queue for consults from any location with a network connection. Previously, no LIS-wide mechanism allowed for determination of where the slide assets resided, either with the primary pathologist or the consultant. The primary pathologist did not know if a consult was finished until the slides and paperwork were back in their mailbox. Deciphering handwriting was also sometimes a time-consuming and error-prone step.
The e-consult system greatly increased the effectiveness of our SP consult system by making all aspects of the process easier. It has become widely accepted amongst faculty with essentially 100% usage for all consultations. Making the process easier makes it more likely that a pathologist will initiate a consult. It is not only easier to initiate a consult but also easier to respond with all the clinical, laboratory, and radiology data from the chart in one place.
The electronic, LIS-based intradepartmental consultation system improves management and documentation of the consultation process. For the primary pathologists, initiating consultations does not require handwriting the tissue site, history, or other information to be passed to the consultant pathologist, as these can easily be gathered electronically. The system allows for tracking of consulted cases. Rather than physically checking a mailbox to see if a consult is finished, this task is facilitated by the pathologist’s individual work queue. For more complex cases which have multiple parts, it is more practical to edit the electronic consultation report, rather than handwriting an extensive reply on a paper form. In some situations, the electronic system provides a simple way to incorporate the consultant pathologist’s reply into the diagnosis line by using the copy and paste function. Although somewhat unexpected, this system prevents time lost attempting to decipher and re-transcribe handwritten text.
For the consultant pathologist, a pending outstanding list for new consults is generated with implementation of the electronic consultation process. This provides immediate awareness of new pending consults and allows an opportunity for consultant pathologists to improve time management. The consultant pathologist is also able to easily see comments from other consultants on the case.
In our department, where we have a hybrid of generalist and specialist practices, we have found the system useful for both types. Diagnoses are increasingly nuanced by more complex data that is continually being added by the literature, and it is becoming more difficult for generalists to be aware of all developments. For pathologists that are on a generalist service, opinions come from subject matter experts, such as those with gynecologic, breast, or gastrointestinal interests or special training. These opinions greatly reduce the chance for misdiagnosis, as they reflect the latest in diagnostic criteria and standards of diagnosis.
For pathologists who are subject matter experts, consultation to another pathologist with expertise in the same area greatly increases the consistency of diagnosis and increases the chance of collaboration on studies that are instigated by an interesting finding in what would be an index case.
We have found the electronic consultations helpful for the management and function of our department in regard to tumor boards. When the physical consultation materials for the cases are requested for conferences or tumor boards, tracking ability provides quick localization of the cases for everybody. This decreases time spent on finding the case materials, which is usually critical before the conferences. Further, an unexpected benefit of having a consultative opinion connected to the report and available to the pathologists involved has been useful when cases are discussed at tumor boards, sometimes long after the report has been issued.
The system has educational benefit for trainees. It is easier for them to track all the steps of the consultation process electronically, as the physical paper forms were not always easily available for them to review. Further benefit was noted for SP fellows in our preliminary diagnosis rotation when providing preliminary diagnoses to clinicians by easily locating the case and accessing the consultation discussion. In addition, ready access to the recorded thoughts of consultants in prior cases can aid in the resolution of diagnostic dilemmas in current cases.
Internal consultation in AP constitutes a significant amount of workload for pathologists.[10] The system provides electronic documentation for all AP consultations and removes the difficulty of performing retrospective reviews of paper-based forms, the need for a physical paper storage area, and clerical time spent on archiving paper consult forms. It also prevents cases from being finalized without formal documentation of consultations. Estimation of workload is performed easily by tallying the number of times an individual pathologist was named in the "Consultants" field. This feature is especially helpful to detect underreported workload for many pathologists. We had no mechanisms to detect undocumented consultations in the paper-based system.
One of the downsides of this system includes the potential for a portion of a consultation discussion to be inadvertently edited or deleted, although we are not aware that this has happened thus far. In addition, it is necessary for the consultant to open the LIS to see the consult question and type his/her reply. Although typing is more efficient than handwriting for most pathologists, some experienced less efficiency with typing.
Conclusion
In summary, our experience of managing intradepartmental consultative activities electronically improved our documentation and operation of the consultation process. It provided tracking ability and facilitated the consultation process for both active and finalized cases by removing paper forms used for consultation. This is a useful tool to improve intradepartmental consultation activities, which have a vital role in preventing misdiagnosis and improving pathology reporting and trainee education.
Acknowledgements
There are no conflicts of interest or financial disclosures.
Authors' contributions
Bilge Dundar contributed to manuscript preparation, data collection, and figure creation. Megan I. Samuelson conceived the project idea and contributed to manuscript editing. Stephanie J. Chen contributed to manuscript editing and figure editing. Anand Rajan KD contributed to manuscript editing, data analysis, and figure creation. John L. Blau, Robert A. Robinson, Michelle L. Greek-Lippe, and Kim S. Lake contributed to manuscript editing.
Competing interests
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
References
- ↑ 1.0 1.1 Gaye, Marema; Mehrotra, Ateev; Byrnes-Enoch, Hannah; Chokshi, Dave; Wallach, Andrew; Rodriguez, Laura; Barnett, Michael L. (21 May 2021). "Association of eConsult Implementation With Access to Specialist Care in a Large Urban Safety-Net System" (in en). JAMA Health Forum 2 (5): e210456. doi:10.1001/jamahealthforum.2021.0456. ISSN 2689-0186. PMC PMC8796905. https://jamanetwork.com/journals/jama-health-forum/fullarticle/2780298.
- ↑ 2.0 2.1 Vimalananda, Varsha G; Gupte, Gouri; Seraj, Siamak M; Orlander, Jay; Berlowitz, Dan; Fincke, Benjamin G; Simon, Steven R (1 September 2015). "Electronic consultations (e-consults) to improve access to specialty care: A systematic review and narrative synthesis" (in en). Journal of Telemedicine and Telecare 21 (6): 323–330. doi:10.1177/1357633X15582108. ISSN 1357-633X. PMC PMC4561452. PMID 25995331. http://journals.sagepub.com/doi/10.1177/1357633X15582108.
- ↑ 3.0 3.1 Ulloa, Jesus G.; Russell, Marika D.; Chen, Alice Hm; Tuot, Delphine S. (1 December 2017). "A cohort study of a general surgery electronic consultation system: safety implications and impact on surgical yield" (in en). BMC Health Services Research 17 (1): 433. doi:10.1186/s12913-017-2375-0. ISSN 1472-6963. PMC PMC5481906. PMID 28645288. https://bmchealthservres.biomedcentral.com/articles/10.1186/s12913-017-2375-0.
- ↑ Kuijpers, Chantal C H J; Burger, Gerard; Al-Janabi, Shaimaa; Willems, Stefan M; van Diest, Paul J; Jiwa, Mehdi (1 October 2016). "Improved quality of patient care through routine second review of histopathology specimens prior to multidisciplinary meetings" (in en). Journal of Clinical Pathology 69 (10): 866–871. doi:10.1136/jclinpath-2015-203488. ISSN 0021-9746. http://jcp.bmj.com/lookup/doi/10.1136/jclinpath-2015-203488.
- ↑ 5.0 5.1 Chen, Bofeng; Talwar, Ruchika; Schwartz, Lauren E.; Terlecki, Ryan P.; Guzzo, Thomas J.; Kovell, Robert C. (1 February 2021). "Second opinion pathologic review in the management of prostate cancer". The Canadian Journal of Urology 28 (1): 10530–10535. ISSN 1195-9479. PMID 33625343. https://pubmed.ncbi.nlm.nih.gov/33625343.
- ↑ 6.0 6.1 Gordetsky, Jennifer; Collingwood, Robin; Lai, Win Shun; Del Carmen Rodriquez Pena, Maria; Rais-Bahrami, Soroush (1 February 2018). "Second Opinion Expert Pathology Review in Bladder Cancer: Implications for Patient Care" (in en). International Journal of Surgical Pathology 26 (1): 12–17. doi:10.1177/1066896917730903. ISSN 1066-8969. http://journals.sagepub.com/doi/10.1177/1066896917730903.
- ↑ College of American Pathologists (22 September 2021). "ANP.10150 Intra and Extra-Departmental Consultations" (PDF). Anatomic Pathology Checklist: CAP Accreditation Program. College of American Pathologists. https://pathology.jhu.edu/campus/CAP-Checklist/Anatomic-Pathology-2021.pdf.
- ↑ Manion, Elizabeth; Cohen, Michael B.; Weydert, Jamie (1 May 2008). "Mandatory Second Opinion in Surgical Pathology Referral Material: Clinical Consequences of Major Disagreements" (in en). American Journal of Surgical Pathology 32 (5): 732–737. doi:10.1097/PAS.0b013e31815a04f5. ISSN 0147-5185. https://journals.lww.com/00000478-200805000-00009.
- ↑ Lueck, Nathan; Jensen, Chris; Cohen, Michael B.; Weydert, Jamie A. (25 April 2009). "Mandatory second opinion in cytopathology" (in en). Cancer Cytopathology 117 (2): 82–91. doi:10.1002/cncy.20019. https://onlinelibrary.wiley.com/doi/10.1002/cncy.20019.
- ↑ 10.0 10.1 10.2 Goebel, Emily A.; Ettler, Helen; Walsh, Joanna C. (1 April 2018). "Intradepartmental consultations in surgical pathology: Review of a standardized process and factors influencing consultation rates and practices in an academic and community hospital setting" (in en). Pathology - Research and Practice 214 (4): 542–546. doi:10.1016/j.prp.2018.02.009. https://linkinghub.elsevier.com/retrieve/pii/S0344033817311925.
- ↑ Renshaw, Andrew A.; Pinnar, Nat E.; Jiroutek, Michael R.; Young, Mary L. (1 May 2002). "Quantifying the Value of In-house Consultation in Surgical Pathology" (in en). American Journal of Clinical Pathology 117 (5): 751–754. doi:10.1309/RD07-39B9-QN1U-L6U0. ISSN 0002-9173. https://academic.oup.com/ajcp/article-lookup/doi/10.1309/RD07-39B9-QN1U-L6U0.
Notes
This presentation is faithful to the original, with only a few minor changes to presentation, grammar, and spelling. In some cases important information was missing from the references, and that information was added. No other modifications were made in accordance with the "no derivatives" portion of the distribution license.